Many women experience changes in their menstrual cycle, pelvic discomfort, or hormonal symptoms at some point in life. When these concerns appear, two conditions frequently come up during medical discussions: ovarian cysts and Polycystic Ovary Syndrome (PCOS).
Because both involve the ovaries and may cause similar symptoms, they are often confused. However, ovarian cysts and PCOS are not the same condition. They differ significantly in their causes, effects on the body, and how they are managed. Understanding the difference is vital for gaining clarity about your reproductive health and hormonal balance.
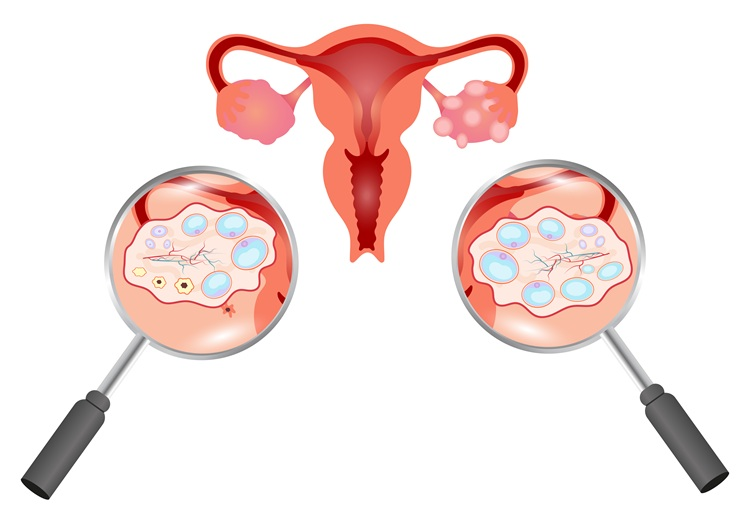
Understanding Ovarian Cysts
An ovarian cyst is a fluid-filled sac that develops on or inside an ovary. Ovaries naturally form small cysts during the menstrual cycle, and in many cases, these cysts disappear on their own without causing any symptoms. However, some cysts grow larger or remain in the ovary for longer periods, potentially causing discomfort.
Common Types of Ovarian Cysts
- Functional cysts: Form as part of the normal menstrual cycle and are usually harmless.
- Dermoid cysts: Develop from reproductive cells and may contain different types of tissue. These have a higher risk of twisting (ovarian torsion) and usually require early surgery.
- Endometriomas: Associated with endometriosis and commonly cause pelvic pain.
- Cystadenomas: Develop from ovarian tissue and can grow quite large. Cysts larger than 5 cm (such as serous or mucinous cystadenomas) are more likely to be pathological and often require surgical removal.
Possible Causes and Risk Factors
Ovarian cysts can develop due to hormonal changes, early or irregular ovulation patterns, endometriosis, or certain ovulation-stimulating medications. You may be more likely to develop them due to your age, hormonal imbalances, a previous history of cysts, or undergoing fertility treatments.
Understanding PCOS
Polycystic Ovary Syndrome (PCOS) is a hormonal condition that affects how the ovaries function. Unlike an isolated ovarian cyst, PCOS involves a broader hormonal imbalance that impacts the endocrine system and several other body functions. It has a strong genetic component and is seen more frequently in women whose mothers had gestational diabetes during pregnancy.
Because hormone levels shift, ovulation may not occur regularly. This can lead to the development of multiple small follicles in the ovaries that look like tiny cysts on an ultrasound.
Common Symptoms of PCOS
- Irregular or missed menstrual periods
- Acne or excessively oily skin
- Excess facial or body hair
- Weight gain or difficulty managing weight
- Thinning hair on the scalp
Ovarian Cyst vs. PCOS: The Key Differences
While both conditions involve the ovaries, their nature and impact are quite different.
| Feature | Ovarian Cysts | PCOS |
| Underlying Cause | Local ovarian changes; often forms as part of the menstrual cycle. | A broader hormonal imbalance affecting ovulation and metabolism. |
| Hormonal Involvement | Hormones play a role, but the condition is usually limited to the ovary. | Strongly linked with systemic hormonal imbalances affecting multiple body systems. |
| Symptoms | Often causes mild pelvic discomfort or remains completely symptom-free. | Causes irregular periods, skin changes, hair growth changes, and metabolic concerns. |
| Impact on Fertility | Usually does not affect fertility unless severe complications occur. | Frequently interferes with ovulation, which can heavily impact fertility. |
| Diagnosis | Typically detected through pelvic examination and imaging tests. | Diagnosed based on menstrual history, symptoms, hormone levels, and imaging. |
| Long-Term Effects | Many cysts resolve naturally without long-term impact. | Requires ongoing management to maintain hormonal and metabolic balance. |
Diagnosis and Management
How Doctors Diagnose These Conditions
If you present with symptoms, a doctor will typically review your medical history, conduct a physical examination, order pelvic imaging (like an ultrasound), and perform blood tests to evaluate your hormone levels.
Treatment Options
Lifestyle Changes for Hormonal Health
Your daily habits play a massive role in maintaining hormonal balance and supporting reproductive health.
- Balanced nutrition: Consuming nutrient-rich foods supports hormonal stability.
- Regular physical activity: Exercise helps maintain metabolic balance. A sedentary lifestyle and weight gain can trigger or worsen PCOS symptoms in genetically predisposed women.
- Stress management: Chronic stress influences hormone levels; relaxation practices are highly beneficial.
- Consistent sleep patterns: Quality sleep supports healthy hormonal regulation.
When to See a Doctor
Do not ignore your body’s warning signs. Seek medical advice if you experience:
- Irregular menstrual cycles lasting for several months
- Ongoing or sudden, severe pelvic pain
- Unexplained bloating or abdominal swelling
- Sudden changes in menstrual bleeding patterns
- Symptoms that interfere with daily life or difficulty conceiving
Frequently Asked Questions
- Can ovarian cysts turn into PCOS?No. Having an ovarian cyst does not mean it will develop into PCOS. They are separate conditions.
- Is PCOS always visible on an ultrasound scan?Not always. Some women have PCOS symptoms even if their ovaries do not show the typical “polycystic” appearance on imaging.
- Do ovarian cysts affect menstrual cycles?Some cysts may temporarily influence menstrual patterns, but many do not cause noticeable changes.
- Are ovarian cysts common in young women?Yes, they are very common during reproductive years and often disappear naturally without complications.
Also Read : PCOS and Fertility Explained: Your Path to Conception